US States Limit Medicaid Coverage for GLP-1 Weight-Loss Drugs Amid Rising Demand
US states drop Medicaid coverage of GLP-1 weight-loss drugs as demand rises
 The Guardian
The Guardian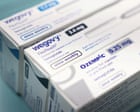
Image: The Guardian
Several U.S. states are cutting Medicaid coverage for GLP-1 weight-loss drugs like Ozempic and Wegovy due to soaring costs, despite rising obesity rates. Legislators warn that this could lead to greater long-term health issues and higher costs for Medicaid recipients. The obesity rate among U.S. adults was 40% in August 2023.
- 01Some U.S. states are restricting Medicaid coverage for GLP-1 weight-loss drugs due to rising costs.
- 02The obesity rate among U.S. adults was 40% in August 2023, with a notable increase in GLP-1 drug usage.
- 03Pennsylvania's Medicaid spending on GLP-1 drugs reached $1.3 billion in 2025, doubling from the previous year.
- 04Legislators argue that cutting coverage may save money in the short term but could lead to higher health costs later.
- 05A proposed subscription model for GLP-1 drugs aims to make them more accessible, but drug manufacturers show little interest.
Advertisement
In-Article Ad
In response to skyrocketing costs, several U.S. states, including California, New Hampshire, and Pennsylvania, are cutting Medicaid coverage for GLP-1 weight-loss drugs, which have seen a 500% increase in spending from $13.7 billion in 2018 to $71.7 billion in 2023. The obesity rate among adults in the U.S. was reported at 40% in August 2023, with 12% of adults taking GLP-1 drugs as of November 2025, a 6% increase from 18 months prior. Critics, including healthcare professionals, argue that these cuts could lead to more severe health issues related to obesity, ultimately increasing costs for Medicaid programs. In Pennsylvania, Medicaid spending on GLP-1 drugs reached $1.3 billion in 2025, prompting officials to limit access based on health criteria. Proposed solutions, such as a subscription model for GLP-1 drugs, face challenges as manufacturers are reluctant to engage. Experts believe that increased competition may eventually lower drug prices, but for now, Medicaid recipients may struggle to access necessary medications.
Advertisement
In-Article Ad
The cuts in Medicaid coverage for GLP-1 drugs may lead to increased health issues among low-income individuals, ultimately resulting in higher healthcare costs for states.
Advertisement
In-Article Ad
Reader Poll
Should states continue to cover GLP-1 drugs under Medicaid despite rising costs?
Connecting to poll...
More about Centers for Disease Control and Prevention
Read the original article
Visit the source for the complete story.







